Algorithm and Techniques for Using Sientra’s Silicone Gel Shaped Implants in Primary and Revision Breast Augmentation
Michael R. Schwartz, MD
Westlake Village, Calif.
Notice of Data Security Incident 10/23/25
Algorithm and Techniques for Using Sientra’s Silicone Gel Shaped Implants in Primary and Revision Breast Augmentation
Michael R. Schwartz, MD
Westlake Village, Calif.


Summary: With the 2006 Food and Drug Administration approval of round silicone gel breast implants in the United States, there still remained a lack of versatility in implant options. The approval of Sientra’s shaped cohesive implants in 2012 brought with it the innovations needed to address varying patient needs. Because access to shaped devices is still fairly recent in the United States, some surgeons remain uncomfortable with implementing shaped cohesive gel implants into their practice. The author outlines surgical techniques and algorithms from experience with the Sientra shaped device, covering the preoperative stage, measurements (base diameter, sternal notch to nipple, tissue pinch, and nipple to inframammary fold), ideal first candidates, operative techniques, and complication avoidance, as well as important factors for shaped-implant selection, including chest base diameter, implant height, implant volume, and implant projection for the patient’s desired outcome. With experience, surgeons will find new utility with gummy bear breast implants for a variety of patients in their practices. (Plast. Reconstr. Surg. 134: 18S, 2014.)
Although 2006 marked the reintroduction of silicone breast implants with improved silicone gel and shell characteristics in the United States, there remained a deficit of implant style options. In comparison, markets outside the United States have enjoyed the option of shaped cohesive implants for over 20 years. In 2012, the Food and Drug Administration approved the Sientra portfolio of Silimed High-Strength Cohesive silicone gel implants, including their HSC+ shaped implants, and ushered in a new and exciting era of breast augmentation options for patients and surgeons in the United States. This article reviews the author’s surgical technique and strategies for complication avoidance with the Sientra HSC+ devices following extensive experience in over 135 consecutive patients for primary and revision cosmetic breast augmentation.
The terms “shaped” and “anatomic” breast implants are typically used to describe nonround devices, designed to shape the breast in a more natural way. These devices are filled with a more cohesive, slightly firmer silicone gel with a higher degree of cross-linking of the silicone polymers compared with traditional round implants. This helps provide the stability required to maintain each implant’s unique shape characteristics while ideally not creating too firm of a result. Each manufacturer has developed its own implant matrices that have variations in height, width, projection, and volume that allow the surgeon to match these characteristics more specifically to each patient’s anatomy and desired outcome.
The currently available Sientra HSC+ implants include 3 footprints: a low-height oval-base implant with high, moderate, and low profiles; a moderate-height round-base implant with a high projection; and a tall-height classic-base implant with a moderate projection.
One distinct advantage of Sientra HSC+ gel implants is the unique blend of soft cohesive gel that combines a more fracture-resistant gel with a strong shell-gel integration, which are intimately bound together. This combination provides an unmatched strength and softness that allows the same surgical control of other shaped devices, yet with a natural, youthful, soft feel. In addition, the safety profile for these devices compares favorably to previous round, less cohesive devices.[1]
Another advantage is related to the TRUE Texture surface. The uniquely textured surface of the Sientra implants provides a balance of traction and adherence to prevent rotation of the implant while still allowing some movement. This also allows for the more form-stable gel of the device to produce controlled tissue expansion over time to shape the breast in patients with a complex anatomy. Finally, it provides long-term stability of the implant pocket, which, in the author’s observation, prevents the “piston effect” of inferior and lateral migration with pectoral muscle movement. Recently published data support the use of shaped textured devices not only for cosmetic enhancement but also as one of the primary controllable factors in the reduction of capsular contracture.[2,3]
The preoperative evaluation of the shaped breast augmentation is the key to a successful outcome (Fig. 1). Shaped implants demand dimensional planning and a detailed and accurate surgeon-patient discussion about objectives and desired outcome. Surgeons should expect to require only 1 or 2 implant options in the operating room as the precise planning, measuring, and pocket dissection essential for a good outcome eliminate the need for several sizes of “backup” implants for each case. Intraoperative sizing is not recommended because it can result in a loose pocket, with inherent risk of rotation or malposition.

The most important measurement is base diameter. It is important to understand that while each patient has a fixed breast base diameter, there is also an ideal postoperative base diameter. Although most surgeons agree with the need to respect the patients’ base diameter, the advantage of a shaped device is the ability to increase this measurement within reason to obtain the result desired by the patient or to correct deformities of the constricted breast.
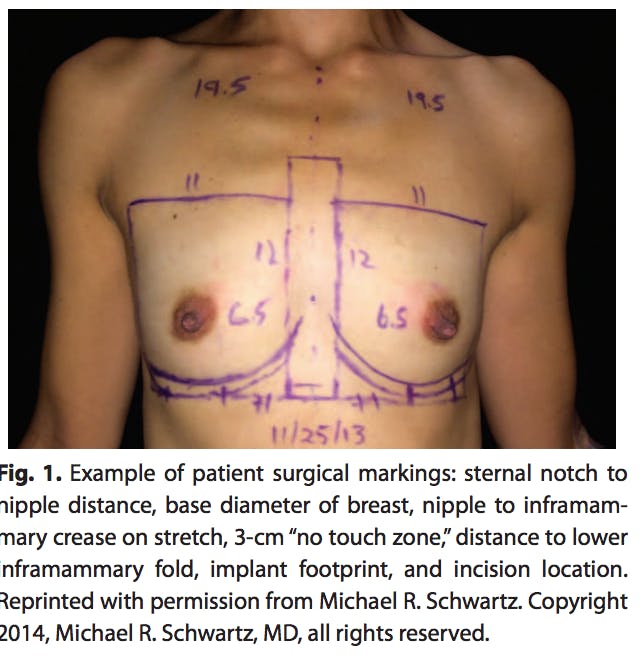
The next measurement is the sternal notch to nipple distance. This is used to select the best implant shape for each patient (Table 1). Patients with a sternal notch to nipple distance 21 cm or greater are best candidates for the taller classic-base implant. Patients with a sternal notch to nipple distance of 18–21 cm are best suited for a round-base device, and patients with a sternal notch to nipple distance less than 18 cm should use a low-height oval-base device. This can be modified based on individual characteristics in each patient’s anatomy including chest wall shape, pectoral muscle development, axillary fullness, and the patient’s implant size choice. For example, a patient with a sternal notch to nipple distance over 21 cm is a candidate for a full-height or shaped classic implant. If the patient has a very full upper chest from either prominent ribs, a well-developed pectoral muscle, or axillary fullness, the surgeon might choose to use a round-base device or even a round implant instead.

The next measurement is the upper-pole tissue pinch thickness. This should be greater than 2 cm if a subglandular plane is being considered. If the tissue pinch thickness is less than 2 cm, the implant should be placed in the submuscular plane. Additionally, each patient should be evaluated for the quality of their skin envelope: loose, tight, or average. This is important to perform at the time of surgical marking for positioning the inframammary incision and pocket dissection.
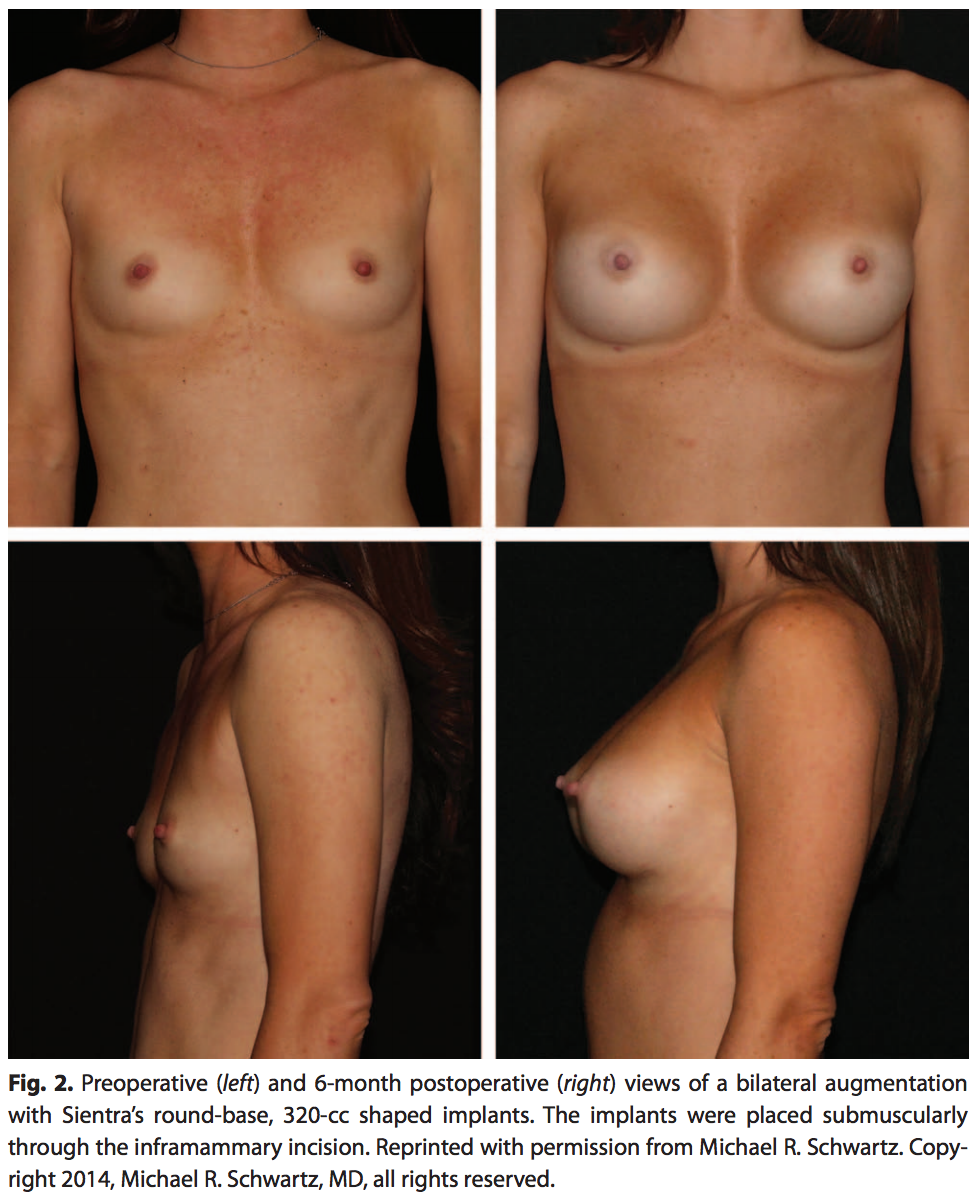
The final key measurement is the distance from the nipple to the inframammary fold on stretch. This measurement is used when marking the patient at the time of surgery to determine the location of the new inframammary fold, if the inframammary fold needs to be lowered for the selected device and incision placement (Table 2). Preoperative measurements are demonstrated in Video 1 (Supplemental Digital Content 1, which demonstrates preoperative measurements, http://links.lww.com/PRS/B7. Used with permission from Michael R. Schwartz. Copyright 2014, Michael R. Schwartz, MD, all rights reserved).
Every algorithm for breast augmentation must include the patient’s size goals. For the author, after the base width and implant shape are determined, there is a discussion with the patient to determine the patient’s size goal. To achieve this, a sizing system can be used, that is, the patient can try on sizers. Another option is to use 3D imaging technology (such as Vectra or Crisalix) to allow patients to visualize the results of different size and shape options, which is a valuable tool for evaluating both size and chest wall asymmetry for surgeons.
Once the implant size has been determined, the final variable is implant projection. This is determined by the 3 variables already selected: base diameter, implant shape, and volume. Each surgeon may prioritize these 4 variables (base diameter, implant shape, volume, and projection) into their own system, using either patient measurements or size goals as their priority. At this time, all manufacturers contain limitations in size and style selection and in available projections, so plastic surgeons will occasionally be required to switch from one type of shaped implant to another (ie, shaped classic to round base or even from a shaped implant to a round implant). In the future, as additional sizes and projections are available in each product line, this will be unnecessary.
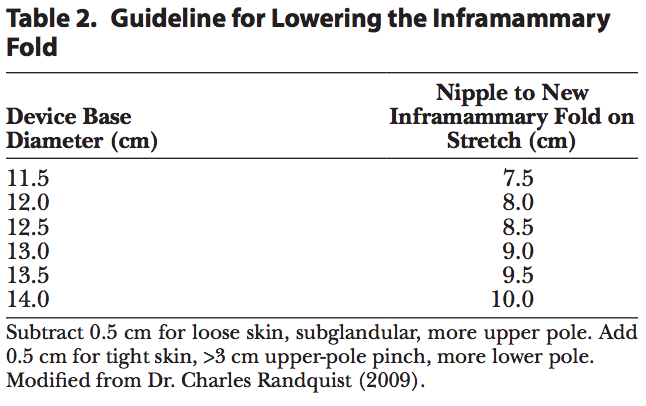

The ideal patient for a shaped implant (Table 3) wants a full but natural result with excellent upper-pole breast shape without the unnatural roundness often seen with round implants (Fig. 2). The patient must be agreeable to a youthfully firm but natural feel. Typically, the implant will be placed through an inframammary incision, both for access and to minimize the risk of capsular contracture.[2–4] Although surgeons may have been reluctant to use the inframammary incision in the past due to visibility of the scar and unpredictable postoperative position, the use of the shaped implant allows accurate incision placement that eliminates these concerns.
As with any cosmetic procedure, it is important to manage patients’ expectations of their surgical result and long-term outcome. Although these implants can produce a very full breast profile, they do not generally result in an “implanted” look, and patients seeking this result should be counseled toward a round device. Despite the natural or “anatomic” shape, these implants cannot be expected to be invisible or not palpable. Complications such as rupture, rotation, double capsule, and seroma have been minimal or absent on both core study data and initial clinical post-approval results.[1] Despite this, patients should be advised that no implant is without potential complications, nor should they be viewed as a permanent device.


There are 4 key measurements in shaped-implant selection: chest base diameter, implant height, implant volume, and implant projection. Breast implant selection is similar to solving a math equation. Each surgeon may select the priorities that fit his or her surgical technique and control 3 of these variables. The fourth is always determined by the other three.
The preference of the author is to use base width as the most important measurement. Base width may vary by 1 cm from the patient’s native breast width (except for extreme breast deformity). The patient may then select the volume she prefers. The surgeon selects the shape of the implant (tall, round, or low height) that fits the patient’s frame. Once these three are selected, the implant projection is predetermined based on these 3 variables.
An alternative is to select the implant based on base width, implant shape, and projection, leaving implant volume as the output variable (ie, the patient does not choose volume). This option allows the surgeon to modify the implant selection process to his or her own style or training or perhaps to each individual patient. This is uniquely different from the past when only a few shapes or size combinations were available.
Preferably, there would be a larger matrix of shaped-implant height and projection combinations from each manufacturer. If the desired implant dimension is not available, the author will switch to an alternate base shape with the appropriate dimensions or a textured round implant.

Patients will start in the supine position with their hands by their side. The author’s personal experience has shown that arms outstretched at 90 degrees distort the pectoral muscle, skin envelope, and breast position and do not allow for accurate implant positioning.
The approach for placing a shaped implant is almost always through the inframammary incision. A shaped implant can be placed through periareolar or axillary incisions, but these approaches are limited to smaller implants and present more difficult dissection.
The ideal location for the pocket is the submuscular or dual plane, which allows sufficient soft-tissue coverage of the implant, while the texturing prevents implant displacement over time. The advantages of the submuscular plane are well known, and recent studies[5] have shown a fairly high complication rate in the subglandular plane and similarly lower complication rate in the submuscular plane.[2,3]
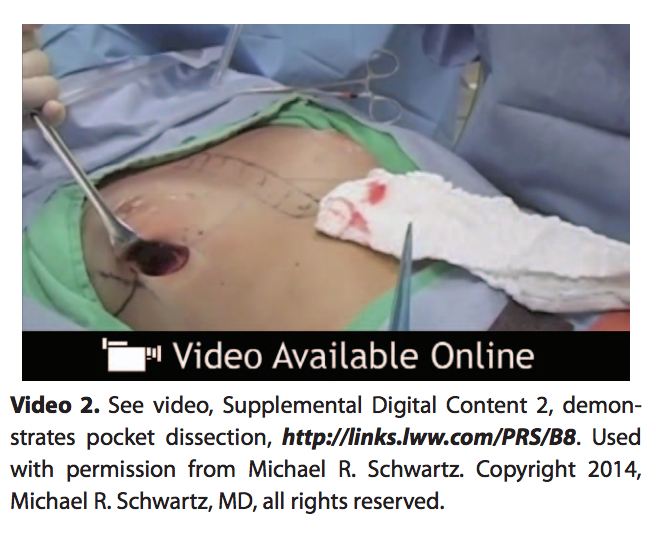
Pocket dissection should be “hand in glove,” with exact preoperative markings and meticulous hemostasis. Monopolar forceps have been found to be the most beneficial tool to acquire for this procedure (Fig. 3). The surgeon may open the optical cavity superiorly first and then define the inframammary fold as marked. Because of the textured and cohesive nature of the implant, the pocket must be opened to the exact shape desired inferiorly and medially to achieve the desired final result. The medial border of the implant pocket is then dissected, taking care to identify and carefully cauterize any vessels noted (See Video 2, Supplemental Digital Content 2, which demonstrates pocket dissection, http://links.lww.com/PRS/B8. Used with permission from Michael R. Schwartz. Copyright 2014, Michael R. Schwartz, MD, all rights reserved). It is appropriate to divide the lateral pectoral insertion only to obtain ideal medial cleavage. The inframammary fold should never be lowered below the initial incision to prevent both bottoming of the implant and a high-riding scar. Digital sweep of the pocket to assess shape is performed. Blunt dissection should not be performed. Sizer implants are used only for breast size or chest wall asymmetry.
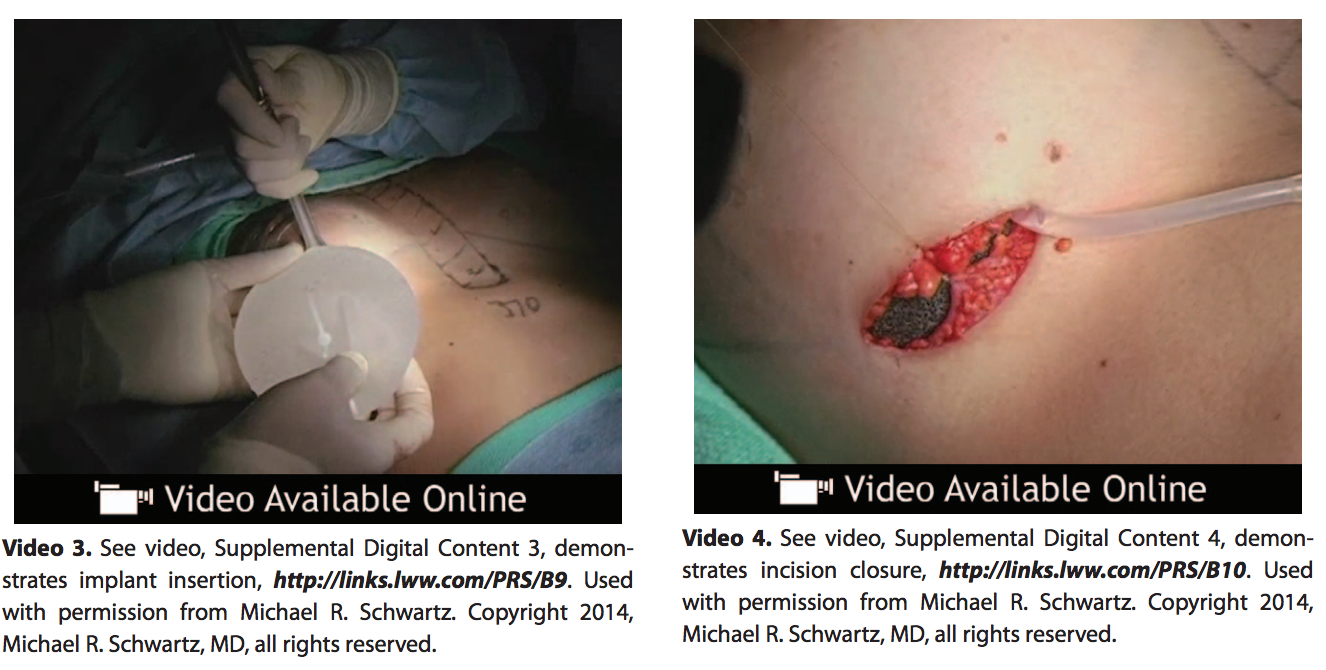
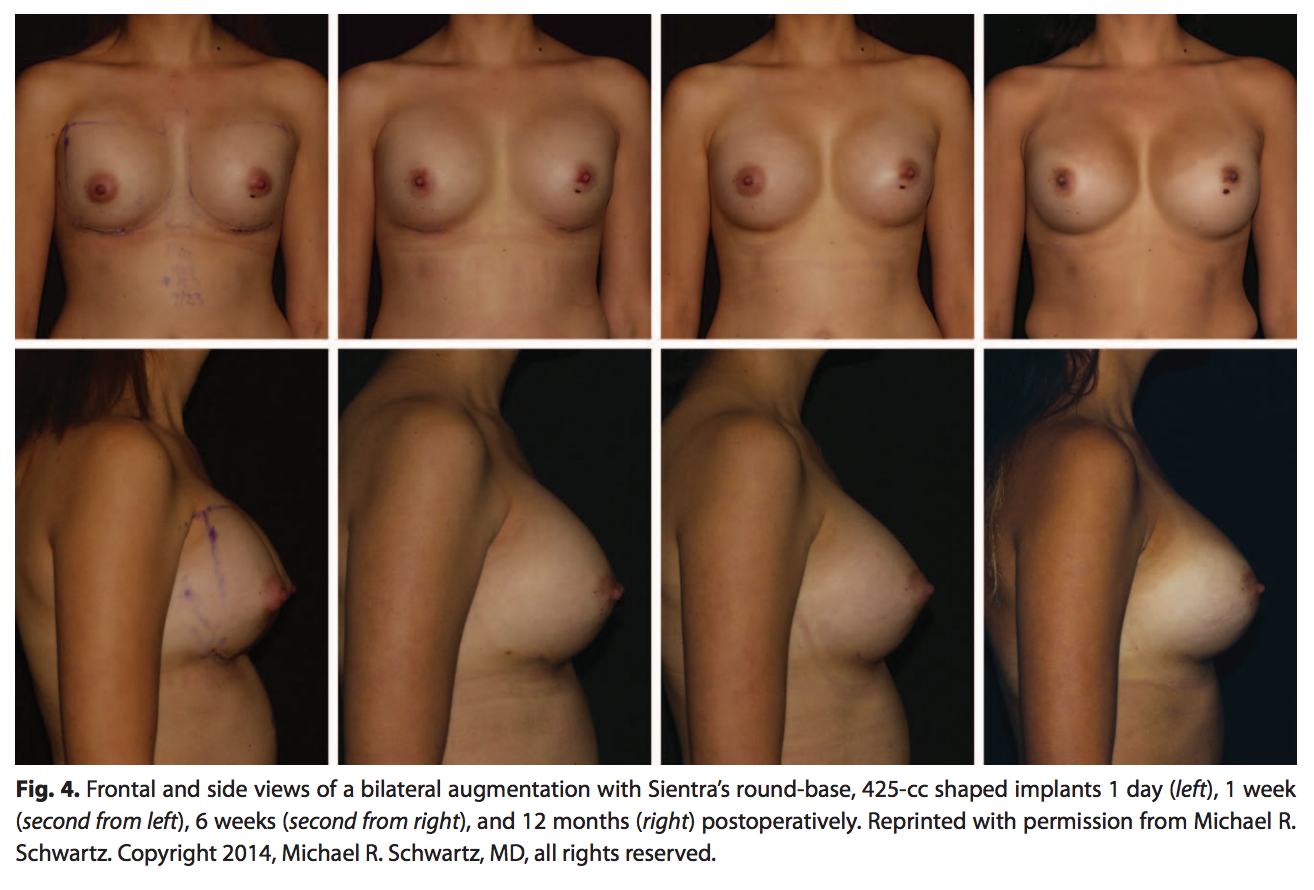
The pocket is irrigated with triple antibiotic solution (Ancef 1 g, Gentamicin 80 mg, and Bacitracin 50,000 U) and then the implant is placed (See Video 3, Supplemental Digital Content 3, which demonstrates implant insertion, http://links.lww.com/PRS/B9. Used with permission from Michael R. Schwartz. Copyright 2014, Michael R. Schwartz, MD, all rights reserved). If there is any shape distortion from placement, it is usually lateral or in the inferior medial border. These 2 areas can usually be released at the completion of the procedure to obtain an ideal final shape. This can safely be accomplished while the implant is in place using good retraction and monopolar cautery dissection. Surgeons who are just beginning to use shaped implants should sit the patient up to assess their result. This is unnecessary as experience is gained. Surgeons should be sure to place the implant in its desired final position. There is no to minimal settling of shaped and/or textured implants postoperatively. Figure 4 depicts an augmentation patient up to 12 months postoperatively with minimal settling.
Marcaine 1⁄4% with epinephrine 1:100,000 is instilled through a fill tube into the implant pocket during incision closure for postoperative analgesia. The incision is closed with 3-0 Monocryl sutures for Scarpa’s fascia and then 4-0 Monocryl and 5-0 Prolene for subcuticular skin closure (See Video 4, Supplemental Digital Content 4, which demonstrates incision closure, http://links.lww. com/PRS/B10. Used with permission from Michael R. Schwartz. Copyright 2014, Michael R. Schwartz, MD, all rights reserved). Deep fascial or chest wall fixation suture is not routinely performed, though it is advocated by some authors.[6] This has not been necessary with the Sientra TRUE Texture surface.
Patients are put in a loose surgical bra to hold the dressing in place only. No compression is applied. They may wear any bra they choose with the exception of push-up bras after their first shower at 48 hours postoperatively. Patients are instructed on stretching the pectoral muscle starting in the recovery room and every hour thereafter on the first day. They are given Toradol intraoperatively and may take any nonsteroidal anti-inflammatory drug of choice immediately postoperatively. They are encouraged to use this alone or in combination with any narcotic analgesic as prescribed.
Patients are encouraged to resume all normal daily activities immediately. They must avoid heart rate elevation for 3 weeks to prevent postoperative bleeding. They may resume limited exercise after 3 weeks and resume all exercises including chest exercises at 6 weeks postoperatively with pain/discomfort as their only guide.
In addition to using these implants in the primary augmentation patient, they have great utility in the patient presenting for revision of prior breast augmentation for multiple indications including capsular contracture, implant malposition, unsatisfactory shape, and symmastia. The control of a shaped textured implant may appropriately address the complication and eliminate the need for more complex and costly techniques such as the use of acellular dermal matrix.

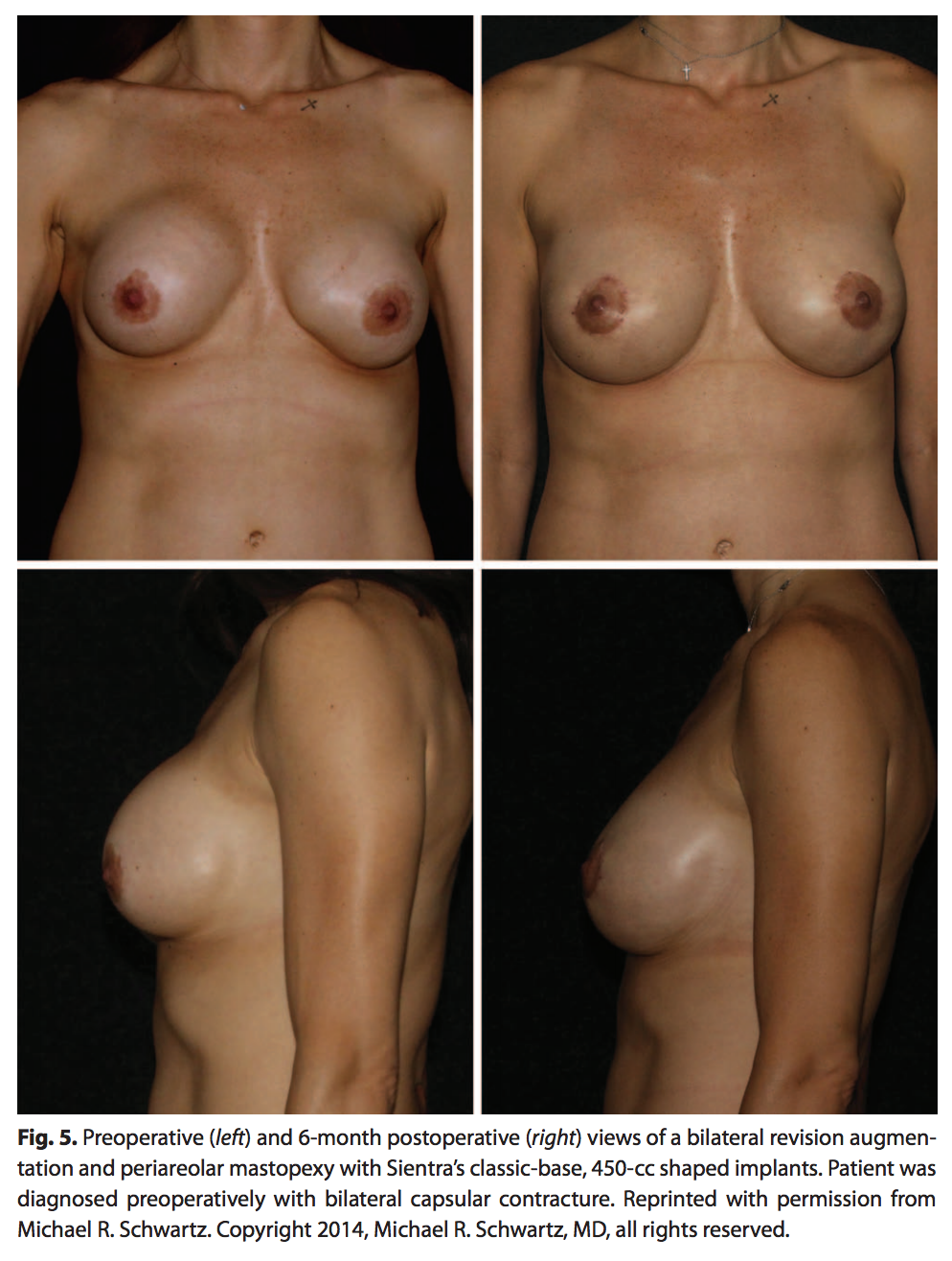
Patients who present with capsular contracture from previous augmentation can be successfully corrected by total capsulectomy and implant replacement with shaped devices. A particular concern in this situation is the loss of control of the pocket size and position when capsulectomy is performed. By taking advantage of the Sientra TRUE Texture surface, closure of the pocket to the appropriate dimension can be accomplished successfully with absorbable sutures such as polydiaxanone sutures or similar ones. This avoids the need for a permanent capsulorrhaphy suture and for acellular dermal matrix support. The author’s preference is to attempt to remove the entire capsule in all patients presenting with capsular contracture. This includes the posterior wall with meticulous dissection and hemostasis. Although this dissection can be difficult and painstaking, it is based on the theory that contracture may be based on bacterial biofilm and leaving the capsule would increase the risk of recurrence. In addition, older implants with increased silicone gel bleed leave microscopic silicone particles, and removing the entire capsule helps to eliminate this additional source of recurrent inflammation and capsule production. All patients undergoing capsulectomy should also be treated with closed suction drainage. Results of an augmentation revision with a preoperative diagnosis of Baker IV capsular contracture are shown in Figure 5.
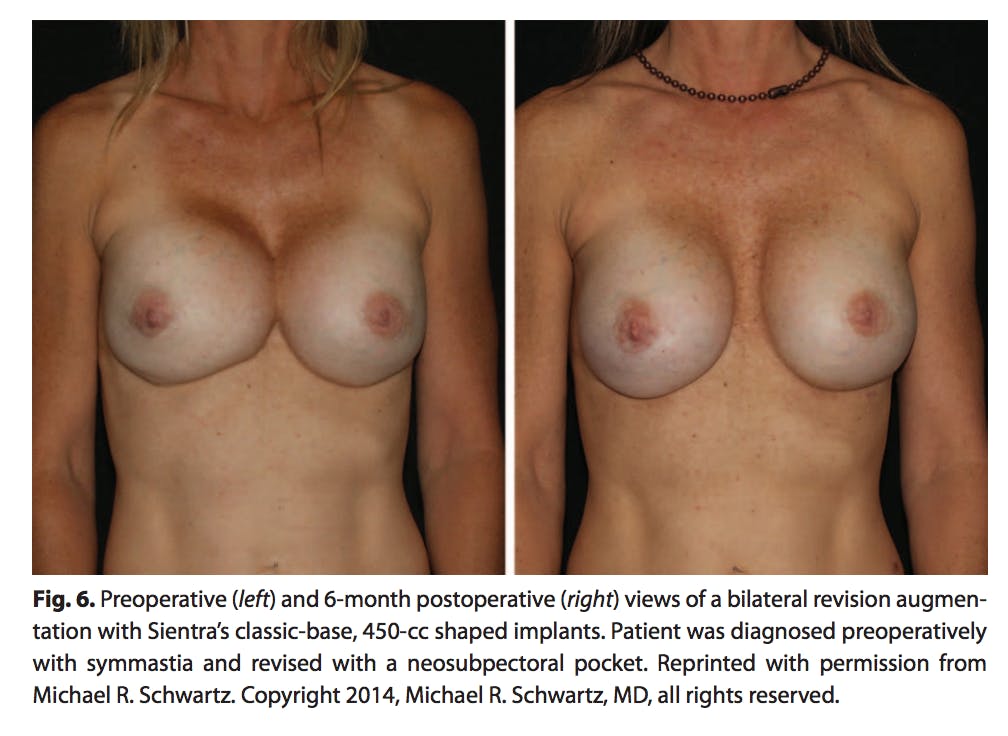
Similar to capsular contracture, the pocket can be modified with absorbable sutures or by using techniques such as a neosubpectoral pocket. Careful dissection to exact pocket dimension will allow successful correction of these deformities with predictable lasting results. In these cases, the pocket is approached through the inframammary incision. The portion of the neopectoral pocket to be created must be carefully planned preoperatively. It is helpful to leave the old implant in place as long as possible to use as a form of traction to help define the new neosubpectoral plane. Initial underdissection is the key. Once the dissection becomes difficult, the old implant pocket is opened at the level of the desired new inframammary fold and the old implant is removed. The old pocket is irrigated with triple antibiotic solution. The author’s preference is to use the “popcorn technique”—electrocautery from inside the old capsule to close any areas that are too large. This avoids sutures that may tear or deform the new neopectoral pocket. A closed suction drain should be left in the old pocket at the time of closure. After the old implant is removed, neopectoral dissection is continued until the new pocket is the exact dimension of the new implant. This presents the perfect opportunity to use the new shaped-implant sizers that are available. Patients should be placed in the upright position to assess pocket shape and position before placement of the final implant. If necessary, absorbable polydiaxanone sutures can also be used to shape the final pocket as necessary. Standard closure is usually acceptable; however, these cases may also require a more aggressive but still absorbable suture in the inframammary fold. All revision patients are required to wear a bra postoperatively for the first 6 weeks. The ideal bra is one that fits the patients comfortably and holds the breast in an appropriate position. It is patient specific, and no single type is ideal. Results of an augmentation revision with a preoperative diagnosis of symmastia using a neosubpectoral plane are shown in Figure 6.
Inherent with many secondary breast surgeries, soft-tissue coverage of the medial implant pocket can be difficult. As has been safely demonstrated, fat grafting can be employed to improve the coverage over any area demonstrating visibility and/or palpability of the new implant.[7] This is ideally scheduled as an elective secondary procedure 3–6 months after the initial procedure to allow the formation of a stable implant capsule and healthy bed for fat grafting. This procedure must be performed in the operating room to protect the sterility of the implant.
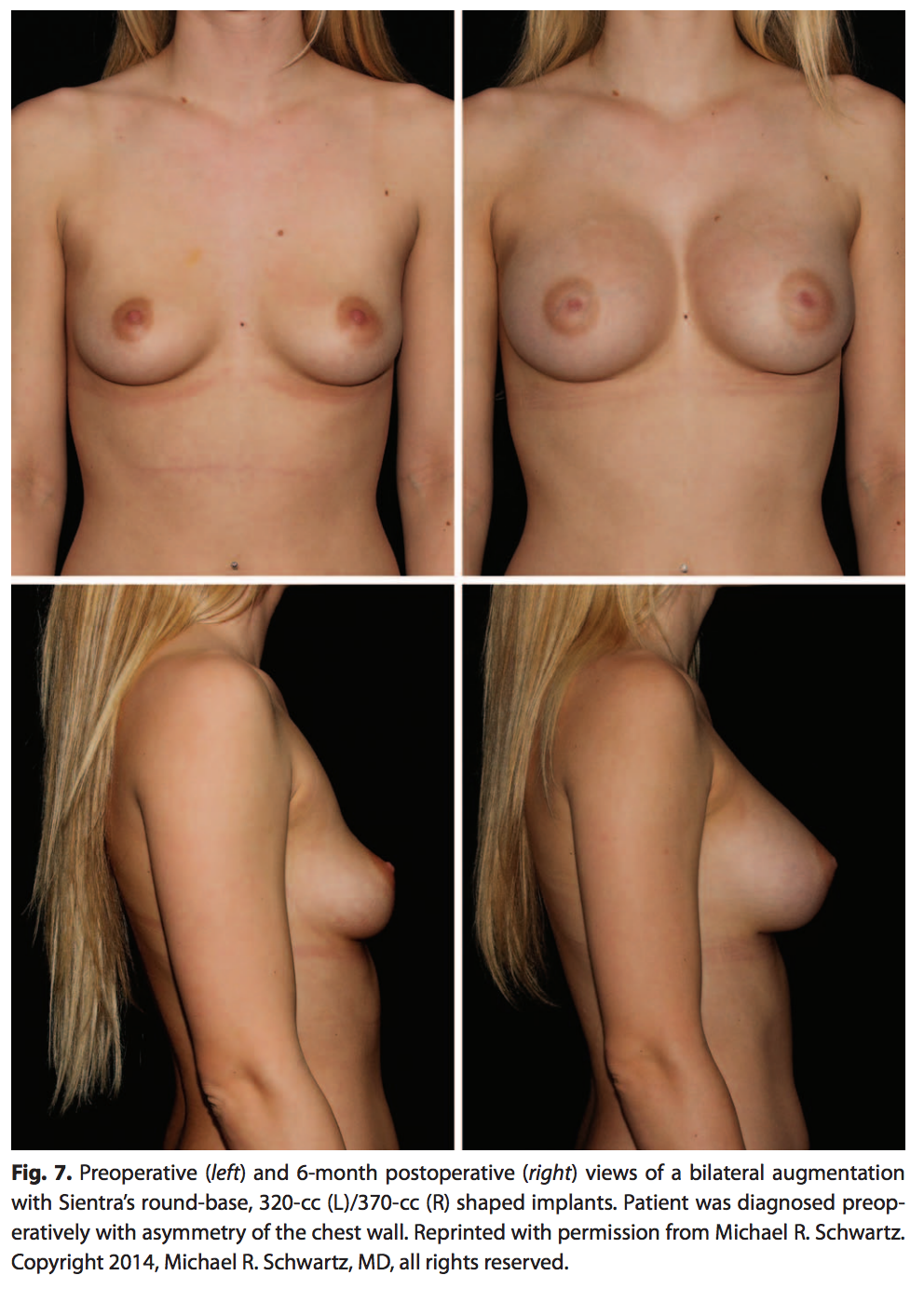
The approval of shaped cohesive breast implants in the United States provides new options to plastic surgeons. However, many plastic surgeons are still hesitant to transition to these new devices. Some await the “ideal” patient to attempt their first case. The ideal patients for any surgeon’s early cases are those who they feel would achieve a great result with their traditional technique as well. The principles provided here will provide a comprehensive basis for success. The experience of a few cases will quickly convince most surgeons of the utility and control of these implants to obtain results in both simple and complex cases (Fig. 7). The experienced use of shaped implants will find new utility with these devices for the patients they have struggled with in the past.
As of March 2012, plastic surgeons in this country finally have the opportunity to use the versatility, options, and control of shaped implants to provide increased refinement in breast augmentation. The ability to select not only diameter and projection but also implant shape further enhances each opportunity to achieve the most patient-specific result every time we enter the operating theater. In addition, the resurgent thinking around form stability and texturing will likely prove to enhance not only the cosmetic result but also patient safety. More careful preoperative evaluation will lead to lower complication rates and enhanced patient satisfaction. In addition, long-term US data are still being collected, and patients should be encouraged to enroll in these postapproval studies to further our collective body of knowledge and contribution to science.

As a solo practitioner with over 120 surgeries completed with shaped implants, the devices were seamless to integrate into my practice and are now the primary device used. It behooves every thoughtful breast surgeon to consider adding shaped highly cohesive implants into their surgical tool kit.
Michael R. Schwartz, MD
Westlake Cosmetic Surgery Center
696 Hampshire Road, Suite 210
Westlake Village, CA 91361
[email protected]
Disclosure: Dr. Schwartz is a clinical study investigator for Sientra and receives standard research support for conducting the study.
If you’re experiencing capsular contracture, please know that you don’t have to live with painful, hardened and distorted breasts forever. We encourage you to schedule a consultation with Dr. Schwartz today for among the best capsular contracture treatment Westlake Village, Thousand Oaks, Calabasas and the greater Los Angeles area have to offer. During that meeting, he will carefully evaluate your breasts while listening closely to your concerns, goals and desired results. From there, he will compose a custom treatment plan designed to resolve any complications and create the ideal chest you’ve always wanted.
Contact Us
© Michael R. Schwartz. All Rights Reserved.
